Also known as DeQuervain’s tenosynovitis, is synovitis or inflammation around the thumb tendons. These tendons sit closely over the bone on the thumb side of the wrist. They run through a firm tunnel and move the thumb away from the rest of the hand.
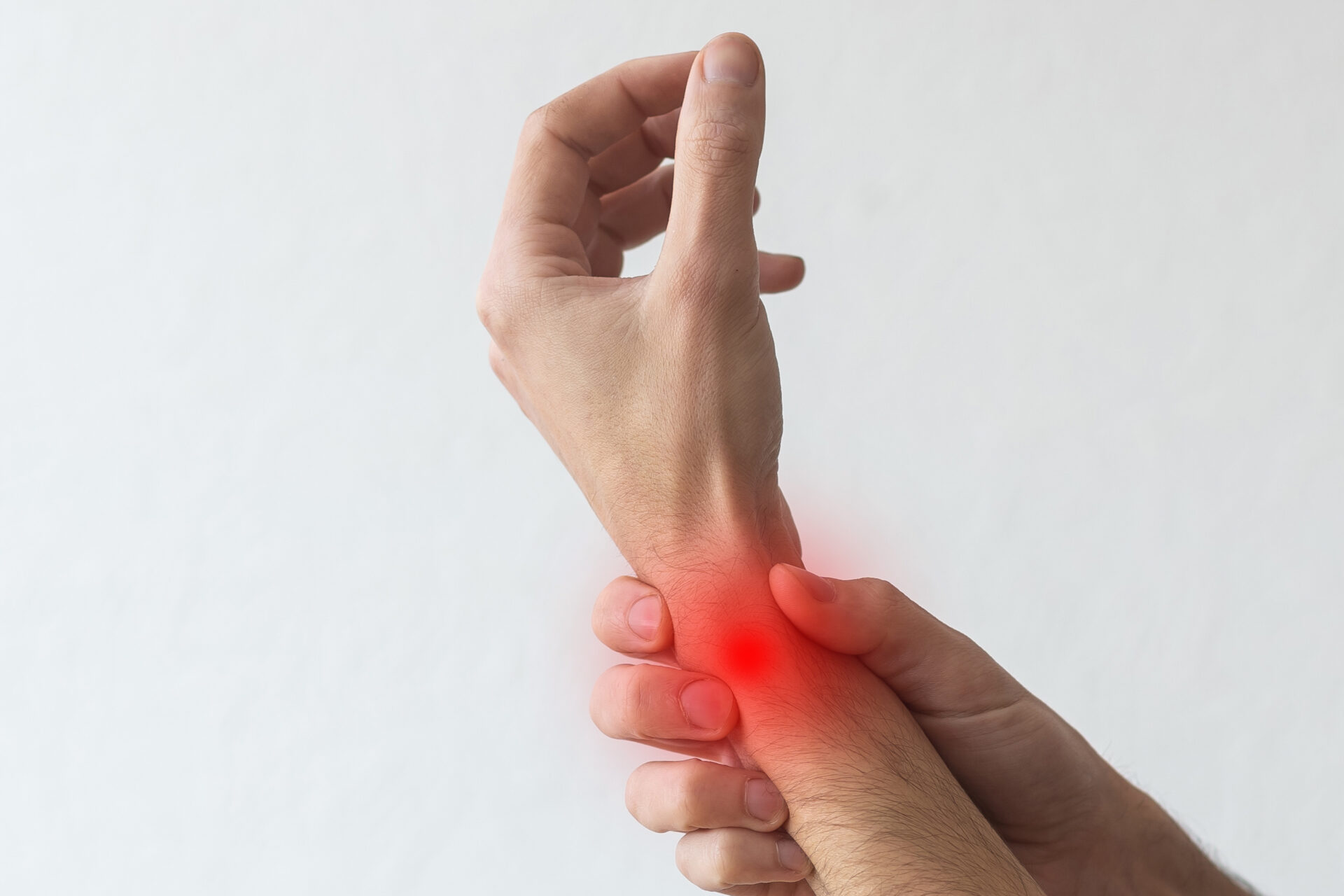
De Quervain’s Disease Treatment
Book AppointmentCauses of De Quervains disease
- Overuse of the hand and wrist
- Inflammatory conditions such as rheumatoid arthritis
- Sharp, direct blow or injury to the thumb
- Repetitive lifting of a newborn
- Secondary to bony abnormalities of the wrist
Symptoms
- Pain and swelling at the base of the thumb
- Tenderness when pressing at the thumb side of the wrist
- Difficulty moving the thumb and/or wrist
- An occasional clicking noise in the tendons
Diagnosis
There is often swelling and inflammation at the thumb side of the wrist. Bending the wrist and thumb towards the little finger leads to pain and confirmation of the diagnosis (Finklestein’s test).
Ultrasound scan or MRI scan may be necessary to confirm the De Quervains diagnosis and the cause of the condition.
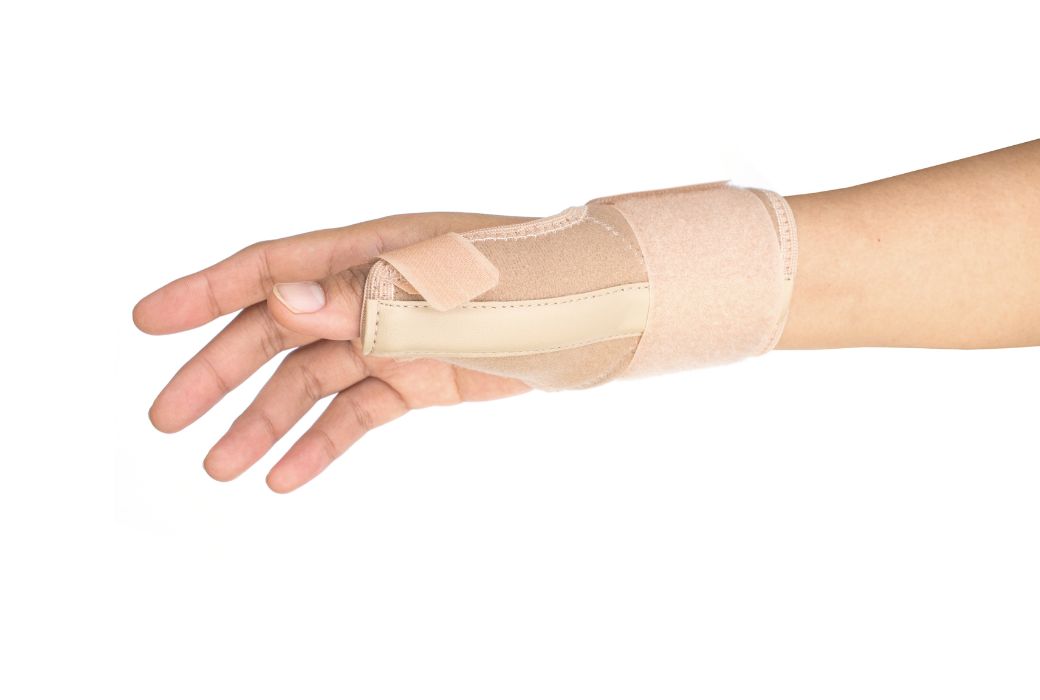
Treatments Available for De Quervains disease
Non-operative treatment
A steroid injection into the tunnel that surrounds the tendons can reduce the inflammation. This can lead to 70-80% success rate when accompanied by hand therapy, splinting and analgesia.
Up to 2 injections can be provided however surgery is advisable for recurrence of the condition.
Operative treatment
The procedure is performed under general anaesthetic through a 3-4 cm incision over the end of the wrist.
The tendon tunnel is reconstructed after removal of the inflammatory tissues at the end of the procedure. Absorbable suture are usually used for the skin.
A bulky dressing is then applied to protect the thumb while the fingers and thumb are free to move.
Sometimes this condition is secondary to an abnormality on the other side of the wrist (ulnar side). In those situations other treatments may be required.
Aftercare and Follow Up
The hand should be kept dry and clean for 2 weeks while the wound heals. One week after the procedure the dressings are reduced by the practice nurse. Hand therapy usually after 48 hours. Normal daily activities and use of the hand is encouraged to avoid tendon and nerve adhesions immediately after surgery. Heavy activity and lifting should be avoided for 6 weeks.

Driving
You should allow a period of approximately 2 weeks before driving and slightly longer if the procedure has been carried out on the left hand side as changing the gear and using the hand break may be difficult to perform.
Time off work
Your return to work will depend on your job. Light manual workers can return to duty in 2 – 3 weeks. Heavy manual workers should not exert maximal grip for 6 weeks.
Scar Desensitisation Exercises
- Circular motion massages to the scar, from the palm moving towards the wrist using a simple moisturising cream. This must be carried out for 10 minutes, at least 3 times a day.
- Rubbing the scar on different textured materials to improve skin sensitivity.
- Submerging the hand under the cold and warm water to improve the temperature sensitivity.

Risks of Surgery
- Infection
- Injury to superficial nerve, blood vessels and tendons
- Scar sensitivity (Scar desensitisation exercises will be arranged by the hand therapist)
- Recurrence
- Failure to resolve all symptoms. 1-2% continue to experience pain and discomfort.
- Further surgery (in event of recurrence or other complications)
- Reduced grip strength
- CRPS (chronic pain syndrome: A small percentage of patients will develop a severe reaction after hand surgery, with lifelong permanent pain and stiffness which requires extensive physiotherapy and pain medication)
Book an appointment
Please use this form if you are interested in booking an appointment. We do not give general medical advice over email.
